
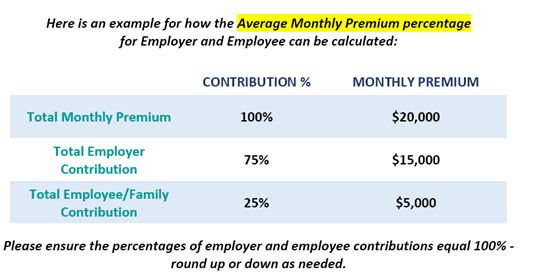
CAA Premium Percentage 2025 Submission
Your Response Is Past Due
See below survey for more guidance on questions.
Please complete immediately.
Survey Question Guidance
|
All Plan Types (Fully-Insured & Self-Funded) |
|
|
Survey Question |
Explanation |
|
Group Health Plan Name: |
This can be found on your invoice or Member ID Card |
|
Group Number: |
This can be found on your invoice or Member ID Card and always starts with “GRP000XXXX” |
|
9-digit employer EIN: |
This is your Employer Identification Number. It can be found in the below documents, or you can contact the IRS. IRS EIN Confirmation Letter (CP 575) Business Tax Documents Call the IRS Tax Line (800-829-4933) |
|
Enter the Average Monthly Premium Paid by Employees |
Per CMS, to calculate the of average monthly premium use total annual premium divided by 12 -- not the average monthly premium on a per-member basis. |
|
Employer Cost Share % |
Employer Cost Share % = Total Premiums Paid By Employer ____________________________ (Total Premiums Paid By Members + Total Premiums Paid By Employer)
Note: Employer Cost Share % + Employee Cost Share % must equal 100 |
|
Employee Cost Share % |
Employee Cost Share % = Total Premiums Paid By Employee ____________________________ (Total Premiums Paid By Members + Total Premiums Paid By Employer)
Note: Employer Cost Share % + Employee Cost Share % must equal 100 |
|
|
If a group health plan submits a Form 5500 to the Department of Labor, enter the 3-digit Form 5500 plan number (self-assigned by the filer in accordance with Form 5500 Instructions). If there is more than one value, separate them with a semicolon.
If you don’t have a Form 5500 Plan Number, leave this field blank.
If you’re not sure if you have a Form 5500 Plan Number, you can look it up using the Form 5500 search tool on the Department of Labor website at https://www.efast.dol.gov/5500search. |
Calculating average monthly premiums
|
Member Premiums |
|
Employer premiums |
||||||
|
Months |
Monthly member premiums |
# of months |
Total member premiums |
|
Months |
Monthly member premiums |
# of months |
Total member premiums |
|
Jan-Dec 2025 |
$6,000 |
12 |
$72,000 |
|
Jan-Dec 2025 |
$10,000 |
12 |
$120,000 |
NOTES: For companies containing multiple policies all policies should be included in the calculation.
Frequently Asked Questions (General)
Q: What is the CAA RxDC Reporting?
A: The CAA RxDC Reporting was established by the Consolidated Appropriates Act (CAA) 2021. It requires health plans to report prescription drug and healthcare cost data to the Centers for Medicare & Medicaid Services (CMS). This data helps CMS understand prescription drug trends and costs.
Q: Is RxDC Reporting mandatory?
A: Yes, RxDC reporting is mandatory for all group health plans, including fully insured, self-insured, and level-funded plans.
Q: Who is responsible for RxDC Reporting?
A:
Fully-Insured Plans: Insurance Carriers are primarily responsible and handle the submission, but they need data (like premium contributions) from the Employer.
Self-Funded Plans: The Employer/Plan Sponsor holds the ultimate responsibility. If the Employer has is contracted with Prominence’s PBM (MedImpact in 2025; Abarca in 2026) Prominence will perform the filing.
If the Employers uses a different PBM, they will work with their PBM to perform the filling.
Q: What is the deadline for submission?
A: Annual submission is due by June 1st for the prior calendar year’s data.
Frequently Asked Questions (Employers/Brokers)
Q: Should premium paid for coverage of an owner of an S-Corporation or Partnership be counted as amount paid by a member or an amount paid by an employer?
A: If the owner works for the business and pays their premium out of personal funds, report the premium as an amount paid by a member.
Q: What if I don’t know the amount of premium paid by Members versus Employers?
A: Section 204 of the CAA, and the Prescription Drug and Health Care Spending interim final rules (86 FR 66662) require premium information to be reported separately according to amounts paid by Members and amounts paid by Employers. Generally, if you are reporting on behalf of a group health plan, you must obtain this information from the plan.
If you are unable to obtain all necessary information to calculate average monthly premium paid by Members and average monthly premium paid by Employers from a plan, you should:
Include the plan when calculating life years, earned premium, premium equivalents, admin fees, and stop-loss premium.